Telehealth Across Borders: A Framework for Multi-State Physician Collaboration
📌 Key Takeaways
Telehealth compliance is determined by where your patient sits during the encounter, not where you hold your primary license.
Physician Licensing Follows Patient Location: Your collaborating physician must hold an active license in every state where patients are physically located during virtual encounters, regardless of where you practice from.
Specialty Alignment Protects Clinical Defense: Using a Family Medicine collaborator for psychiatric telehealth creates liability gaps that undermine your defense if patient outcomes are challenged.
Chart Review Requirements Vary Significantly: Jurisdictions range from strict percentage mandates to periodic quality meetings without fixed counts; build workflows that meet the strictest standard across all active states.
Coverage Gaps Require Immediate Legal Counsel: Practicing during a collaboration gap is viewed as operating outside scope; retroactive chart review does not cure the lapse, though good-faith remediation may mitigate disciplinary consequences.
Regional Patient Concentration Drives Infrastructure Planning: Most out-of-state patients originate from immediate neighboring jurisdictions, allowing strategic investment in high-value state coverage rather than scattered expansion.
Map locations, verify licenses, update agreements—systematic preparation transforms expansion from regulatory crisis to predictable growth.
Independent Nurse Practitioners scaling virtual practices across state lines will find a clear compliance framework here, preparing them for the jurisdictional challenges detailed in the implementation roadmap that follows.
~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~
From Single-State Practice to Multi-State Compliance Confidence
The patient intake form loads. State of residence: Ohio. You freeze. Your collaborating physician isn't licensed there.
This moment—the realization that your virtual practice has outgrown your compliance infrastructure—is becoming increasingly common for independent Nurse Practitioners. You built a thriving telehealth practice in your home state, but now patients from neighboring states are requesting appointments. Each new state represents both an opportunity and a potential regulatory minefield.
State-licensed physician oversight ensures NPs meet local practice mandates in specific jurisdictions. Think of it like a local guide who knows the terrain: it allows you to practice with the certainty that you are fully compliant with a specific state's complex medical board rules.
Executive Summary
The Core Challenge: Independent NPs expanding telehealth services into Reduced or Restricted Practice states face a jurisdictional compliance gap. In these jurisdictions, state law requires physician oversight in the state where the patient is physically located, not just where the NP holds their primary license.
The Solution Framework: A systematic multi-state collaboration strategy that identifies patient location trends, secures licensed physician partners in each jurisdiction, and updates Collaborative Practice Agreements to reflect telehealth-specific oversight requirements.
The Business Value: This framework transforms regulatory expansion from a reactive crisis (triggered by a surprise audit) into a predictable growth process that protects your prescriptive authority and practice legitimacy across state lines.
The Jurisdictional Reality: Compliance Follows the Patient
Here's the principle that catches most NPs off guard: telehealth compliance isn't determined by where you sit during the video call. It's determined by where your patient sits.
Think of state-specific physician collaboration as hiring a local guide. When you hike in unfamiliar terrain, you don't bring a guide who only knows the trails back home. You need someone who knows the specific territory you're entering—the regulations, the common pitfalls, the exact requirements of that jurisdiction.
State-Specific Physician Collaboration prevents Regulatory Non-Compliance by ensuring your supervising physician holds an active, current license in every state where you treat patients. This isn't just a best practice—it's a legal requirement in most jurisdictions. A Pennsylvania-licensed collaborator cannot provide the oversight required for a patient receiving care in Ohio, even if you're both on a video call.
Why Multi-State Licensure Isn't Automatic
Many NPs assume that if they hold licenses in multiple states through the Nurse Licensure Compact, their collaborating physician can provide oversight across those same states. This is incorrect. Physician licensure doesn't work the same way. Your collaborator needs individual state medical licenses for each jurisdiction where they'll be providing supervision—and those licenses must be active and in good standing.
Key Terminology:
Collaborative Practice Agreement (CPA): The legal contract defining the NP-Physician relationship, including scope of practice, chart review frequency, and communication protocols.
Prescriptive Authority: Your legal ability to prescribe medications, which is directly tied to having proper physician oversight in the patient's state.
Cross-State Licensure: The requirement that physicians hold individual state licenses (not reciprocity) for supervision purposes.
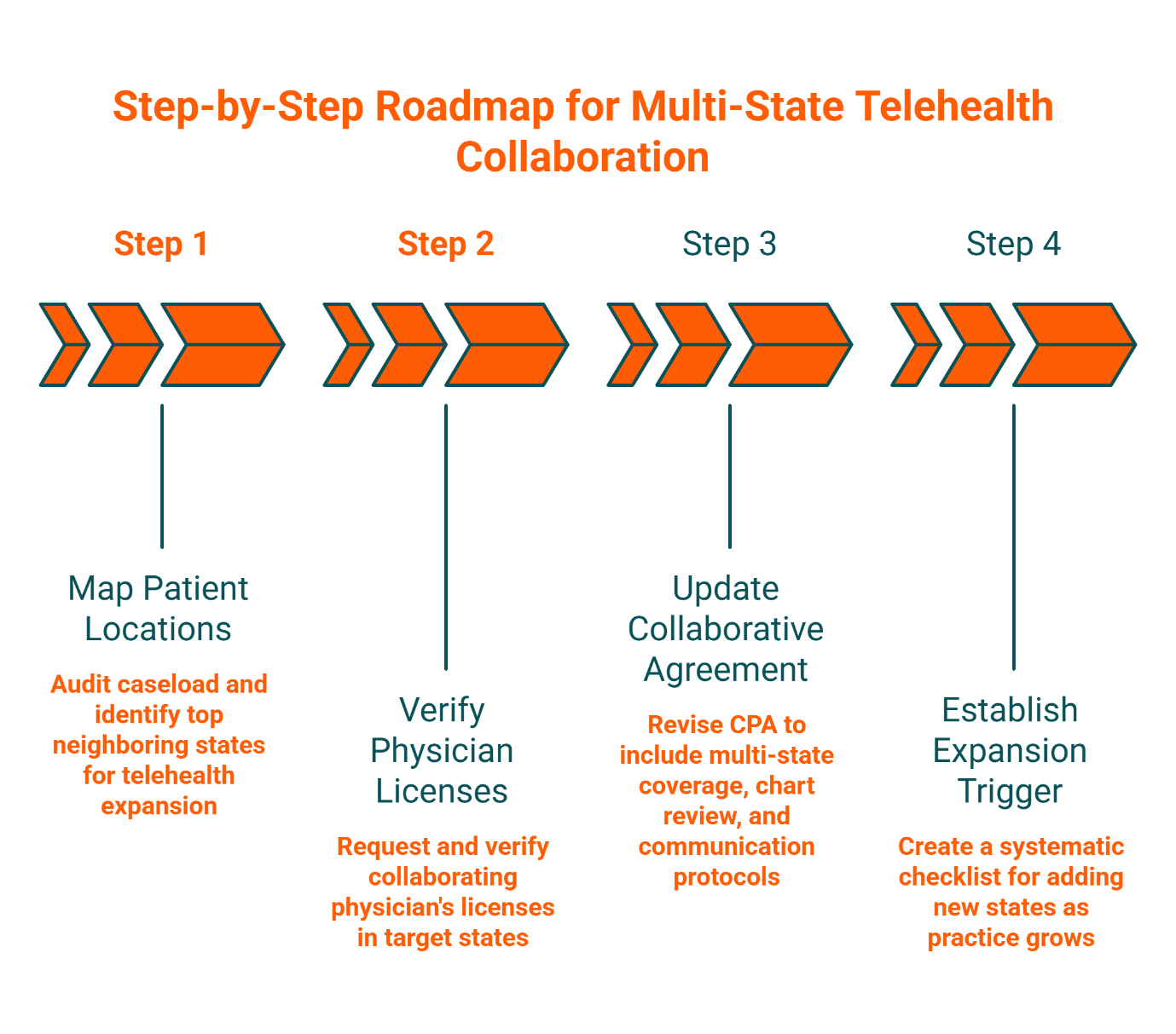
A Step-by-Step Roadmap for Multi-State Telehealth Collaboration
Partnering with multi-state supervising physicians enables expansion by providing access to a network of licensed physicians across multiple jurisdictions. Here's how to build your compliant infrastructure:
Step 1: Map Your Patient Location Data
Before you can build the right compliance framework, you need to know where your patients actually are.
Audit Your Current Caseload: Pull your patient database and identify the states where patients are physically located during appointments. Don't just look at billing addresses—verify where they're receiving care.
Identify Your Top Neighboring States: Industry observations suggest that a significant concentration of out-of-state patients typically originates from immediate neighboring jurisdictions, driven by regional marketing and referral patterns.
Project Your Growth: If you're marketing to a regional audience, which states are you likely to add next?
This data-driven approach prevents you from over-investing in coverage for states where you rarely see patients while ensuring you're protected in the jurisdictions that matter most to your practice.
Step 2: Verify Physician License Parity
Once you know which states you need coverage in, it's time to audit your collaboration network.
Request License Verification: Ask your current collaborating physician for their active state medical licenses. Verify these against the states where you're seeing patients.
Identify the Gap: For each state where you treat patients but your physician isn't licensed, you have a compliance gap that needs to be addressed.
Evaluate Specialty Match: This is especially critical for specialized practices. If you're providing psychiatric telehealth, your collaborating psychiatrist should be board-certified in psychiatry—and that certification should be valid in each state where you practice.
Step 3: Update Your Collaborative Practice Agreement for Telehealth
A Collaborative Practice Agreement secures Telehealth Prescriptive Authority, but only if it's written to account for the unique requirements of virtual care.
Your CPA should explicitly address:
Multi-State Coverage: List each state where the agreement applies and confirm your collaborator holds an active license in all listed jurisdictions.
Chart Review Protocols for Virtual Encounters: Specify how often charts will be reviewed. Requirements vary significantly by jurisdiction, ranging from strict percentages (e.g., 10% of charts) to periodic quality improvement meetings (e.g., monthly or quarterly) without fixed chart counts.
Telecommunication Methods: Define approved communication channels (encrypted messaging, phone, video) for consultations and questions.
State-Specific Prescribing Limits: If a state has unique restrictions on controlled substances or telemedicine prescribing, document those limitations clearly.
Step 4: Establish Your Expansion Trigger Process
Build a systematic process for adding new states as your practice grows:
The Telehealth Expansion Checklist:
☐ Patient requests appointment from a new state
☐ Verify state allows NP telehealth practice
☐ Confirm you hold an active NP license in that state
☐ Check if current collaborator is licensed there
☐ If not, initiate search for state-specific collaborator
☐ Update CPA to include new jurisdiction
☐ Verify malpractice coverage extends to new state
☐ Update patient intake forms to reflect expanded service area
☐ Train staff on state-specific documentation requirements
This checklist transforms expansion from a reactive scramble into a predictable 30-day process.
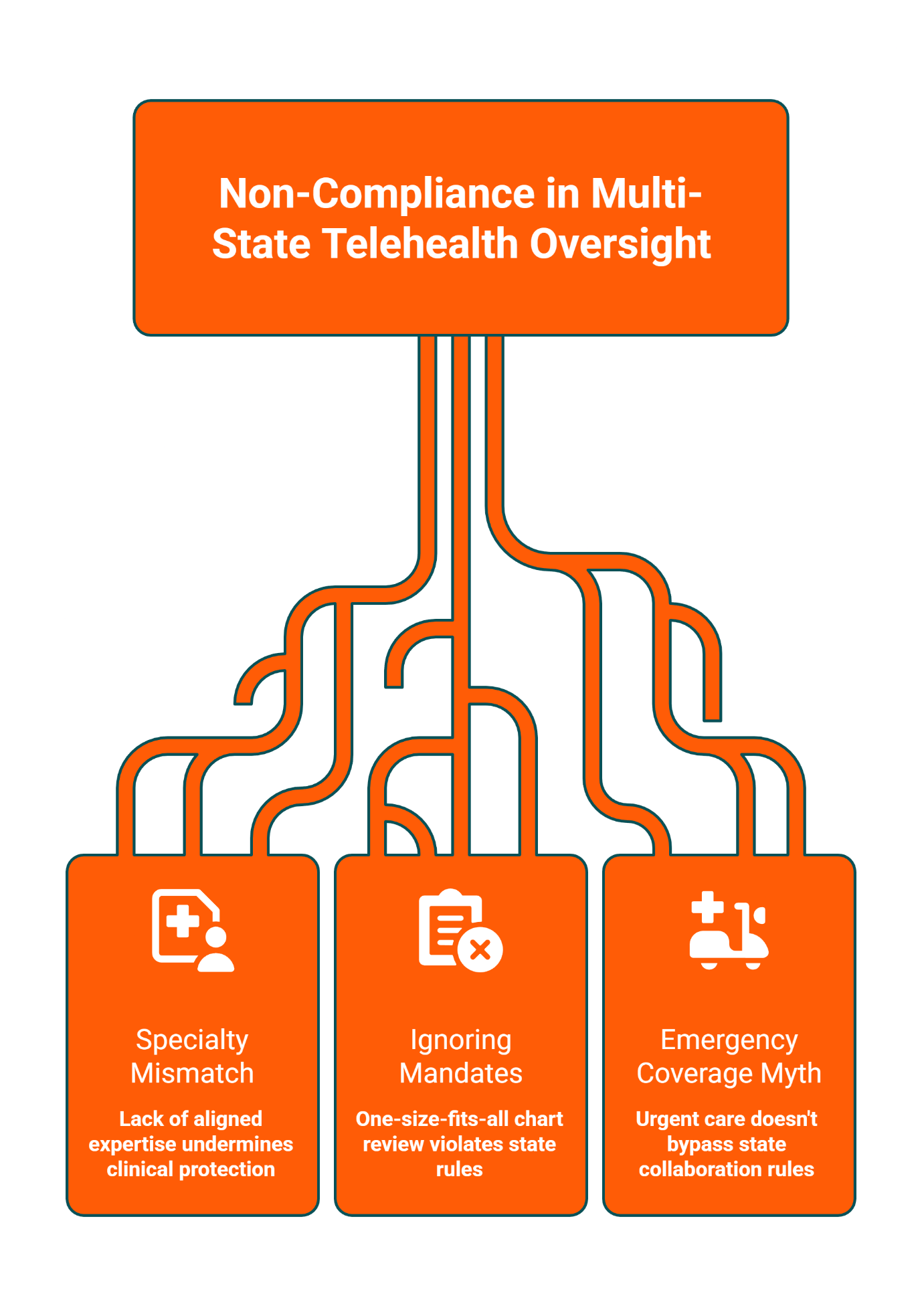
Common Pitfalls to Avoid in Virtual Oversight
Pitfall 1: Specialty Mismatch in Secondary States
Picture this: You're a Psychiatric Mental Health NP. Your primary collaborator in Pennsylvania is a psychiatrist. You expand to New Jersey and secure a Family Medicine physician as your collaborator there because they were faster to onboard.
This creates a liability gap. While it might technically satisfy the "physician supervision" requirement in New Jersey, it doesn't provide the specialty-aligned oversight that protects you clinically. If a patient in New Jersey files a complaint about psychiatric care, and your collaborator isn't trained in psychiatry, you've undermined your own defense.
The Fix: Maintain specialty alignment across all states. If you practice behavioral health, all your collaborating doctors should be psychiatrists or have documented expertise in mental health.
Pitfall 2: Ignoring State-Specific Chart Review Mandates
Chart review frequency isn't universal. Some states require monthly reviews of a specific percentage of charts. Others mandate quarterly reviews but with stricter documentation requirements. A few states require synchronous (real-time) chart review for certain controlled substances.
If you're using a one-size-fits-all chart review process across multiple states, you're likely non-compliant in at least one jurisdiction.
The Fix: Maintain a compliance matrix that lists each state's specific chart review requirements and build your documentation workflow to meet the strictest standard across all your active states.
Pitfall 3: The "Emergency Coverage" Myth
Some NPs believe they can treat out-of-state patients "temporarily" without proper oversight if it's clinically urgent. This is incorrect. Emergency exceptions exist for physicians treating patients across state lines during disasters, but these exceptions don't extend to routine NP telehealth practice.
Every patient encounter—urgent or routine—must meet the collaboration requirements of the state where the patient is located at the time of the encounter.
Scaling Your Virtual Infrastructure Compliantly
As your practice grows, you'll need to make a strategic decision: Do you want to manage multiple individual collaboration agreements across states, or do you want to partner with a collaborative physician network that already has multi-state coverage built in?
For practices serving patients in 1-2 states, individual agreements often work well. You have direct relationships, clear communication, and straightforward overhead.
For practices serving patients in 3 or more states—or for NPs planning aggressive geographic expansion—a collaboration network offers significant advantages. These services maintain rosters of licensed physicians across dozens of states, allowing you to add new jurisdictions in days rather than months. When a patient from a new state books an appointment, the network can often assign you a collaborator in that state within a week.
The key is understanding what you're scaling toward. If your vision is a regional telehealth practice serving 5-7 neighboring states, plan for that infrastructure now rather than scrambling to patch together agreements reactively.
What If You Discover a Coverage Gap Mid-Practice?
Let's address the scenario that keeps practice owners up at night: You've been seeing patients in a state where you thought you had proper coverage, but a surprise state board inquiry reveals your collaborator isn't licensed there.
First, don't panic. This situation is more common than you think, and it's often resolvable.
Your immediate action plan:
Pause new patient encounters in the affected state until you secure proper coverage.
Notify your malpractice carrier immediately. They need to know about the potential exposure.
Secure a properly licensed collaborator in that state as quickly as possible.
Consult legal counsel immediately regarding remediation. While you must secure a new collaborator instantly, do not assume retroactive review cures a lapse. Most state boards view practice during a gap in collaboration as practicing outside of scope. However, demonstrating a good-faith effort to audit past cases for safety may be a mitigating factor during disciplinary proceedings.
Document everything. Create a clear timeline showing when you discovered the gap and how quickly you remediated it.
The severity of the consequences depends heavily on how you respond. State boards distinguish between NPs who operated recklessly versus those who made a good-faith error and immediately corrected it. Your transparency and speed matter.
Expert Q&A: Specialty Alignment Across State Lines
Question: "Is it legal for a Family Medicine doctor to supervise my Psychiatric telehealth practice if the patient is in a different state?"
Answer: While laws vary, state boards increasingly require specialty-matching for clinical credibility. Using a generalist for a specialized telehealth practice creates a liability gap in most jurisdictions. Even if it's technically "legal" under a loose interpretation of the supervision statute, it undermines your clinical defense if a patient outcome is challenged. The standard you should aim for isn't "what's technically allowed" but "what creates the strongest foundation for safe, defensible care." For psychiatric practice, that means working with collaborators who have psychiatric training or documented mental health expertise.
Resources
Your Path to Confident Multi-State Practice
You started your independent practice because you wanted autonomy—the freedom to practice medicine on your terms, serve the patients who need you most, and build a business that reflects your values.
Multi-state telehealth expansion is the natural evolution of that vision. It's not just about seeing more patients or generating more revenue. It's about practicing with the confidence that comes from knowing your infrastructure can support your ambition without exposing you to regulatory risk.
The framework outlined here—mapping patient locations, verifying license parity, updating agreements, and building systematic expansion processes—transforms telehealth growth from a source of anxiety into a predictable path forward. You're not just adding states to your service area. You're building a practice that can scale safely, sustainably, and compliantly across jurisdictions.
That's the difference between a practice that's constantly reacting to compliance crises and one that's confidently serving patients wherever they are.
Disclaimer: This article provides general information about multi-state telehealth collaboration requirements for educational purposes. State laws governing NP practice and physician oversight vary significantly and change frequently. This content does not constitute legal or regulatory advice. Before expanding your practice across state lines, consult with a healthcare attorney familiar with the specific regulations in each jurisdiction where you plan to practice.
Our Editorial Process
Our expert team uses AI tools to help organize and structure our initial drafts. Every piece is then extensively rewritten, fact-checked, and enriched with first-hand insights and experiences by expert humans on our Insights Team to ensure accuracy and clarity.
About the Physician Collaborators Insights Team
The Physician Collaborators Insights Team is our dedicated engine for synthesizing complex topics into clear, helpful guides. While our content is thoroughly reviewed for clarity and accuracy, it is for informational purposes and should not replace professional advice.