Emergency Compliance: How to Secure a Supervising Physician Fast Before Your Practice Opening
📌 Key Takeaways
A missing collaborating physician is the single biggest obstacle to your practice opening—but you can fix it in seven days with the right approach.
Start Your State Board Research Now: Your state's nursing board website tells you exactly what oversight you need before you can prescribe, bill insurance, or legally open your doors.
Prepare Your Information Packet First: Gathering your license, malpractice coverage, practice type, and NPI number before reaching out speeds up every conversation and shows you're serious.
Speed Without Vetting Creates Bigger Problems: A quick signature from the wrong physician—someone in the wrong state, wrong specialty, or never available—can trigger license-threatening audits later.
Match Timing Is Faster Than You Think: Quality collaboration services typically match NPs with physicians within one week, with quotes returned in 24 hours.
Flexibility Protects You Long-Term: Choose arrangements that let you switch physicians if the fit isn't right—being locked in creates liability when things change.
The right collaboration isn't just paperwork—it's the foundation your entire practice stands on.
Nurse practitioners launching independent practices will find a clear roadmap for securing compliant physician oversight quickly, preparing them for the detailed seven-day sprint that follows.
~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~
The calendar shows your grand opening circled in red. Fourteen days out. The space is leased, the equipment ordered, and the patient scheduling software finally configured. But the credentialing form sits on your desk with one line conspicuously empty: the supervising physician signature.
A supervising or collaborating physician, depending on your state's terminology, is the licensed doctor who provides oversight for your nurse practitioner practice as required by state law. Think of this relationship less like hiring an employee and more like securing the legal foundation that allows your entire building to stand. Without it, even a fully built practice cannot open its doors.
This scenario plays out across the country every month. An NP founder pours months of work into launching an independent practice, only to realize in the final weeks that payer enrollment cannot proceed, prescriptive authority cannot activate, or the state board application cannot move forward—all because physician oversight documentation remains incomplete. The practice that was supposed to open in two weeks now faces an indefinite delay.
The good news: this bottleneck is entirely preventable. With the right preparation and a structured approach, you can secure compliant physician collaboration in as little as seven days. This guide walks you through exactly how to do it—without cutting corners that create bigger problems later.
Ready to start the process now? Get a free quote and receive a response within 24 hours.
Your Grand Opening Can Stall Before You See Your First Patient
The payer enrollment packet sits in a digital queue. The state board email remains unopened because you already know what it says: documentation incomplete. These are the moments when the reality of physician oversight requirements stops being abstract regulatory language and becomes the single obstacle between you and revenue.
For nurse practitioners in states with reduced or restricted practice authority, collaboration is not optional. It is an opening dependency. Your ability to prescribe medications, bill insurance, and legally operate hinges on having a properly documented relationship with a licensed physician. The AANP's State Practice Environment map outlines where these requirements apply, but the operational impact is consistent: no collaboration agreement means no practice launch.
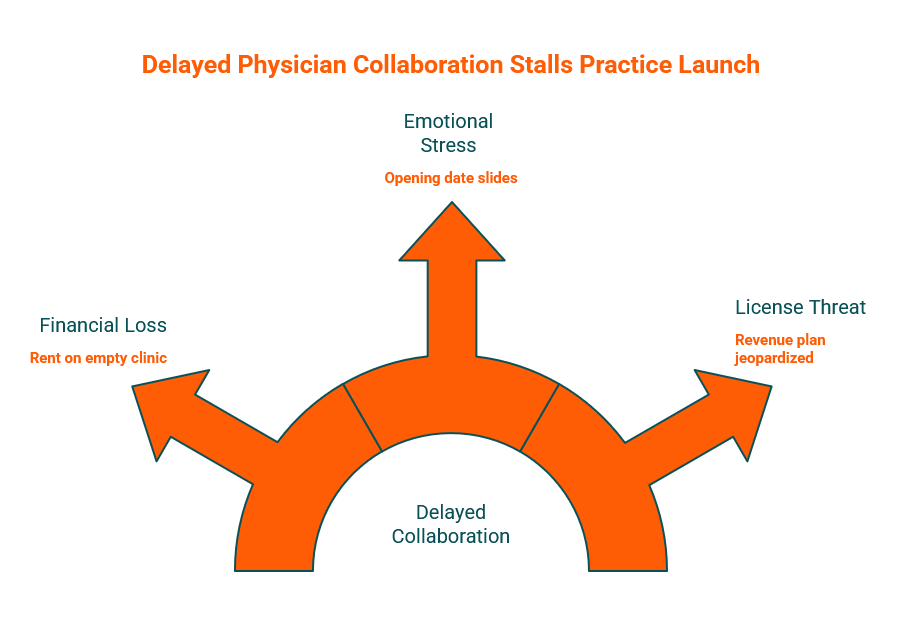
The financial stakes compound quickly. Every week of delay means rent paid on an empty clinic, staff waiting without patients, and the marketing momentum you built quietly dissipating. Beyond the dollars, there is the emotional weight. You did not leave a stable position to become an independent practice owner only to watch your opening date slide because of paperwork.
Healthcare compliance dependencies rarely fail gracefully. They tend to surface at the worst moment, when other launch costs are already committed and the margin for error is thin. A late search for a supervising or collaborating physician creates stress beyond paperwork—it can threaten the launch date, the license posture, and the revenue plan all at once.
This is not about regulatory technicalities. This is about business survival.
What "Emergency Compliance" Really Means for an NP Practice Launch
Emergency compliance is not about panic. It is about compressing a process that typically takes weeks into a focused sprint that protects your timeline without sacrificing due diligence.
Think of physician collaboration as a legal shield and a launch system at the same time. It protects the practice from fragile shortcuts, and it gives the business a structure that can withstand scrutiny. The right physician relationship becomes the infrastructure of independence—not a box to check on the way to opening, but the foundation that supports everything else.
The phrase "supervising physician" or "collaborating physician" refers to the licensed doctor who provides oversight for your practice according to your state's nurse practitioner regulations. In some states, this involves a formal Collaborative Practice Agreement (CPA) that specifies scope, chart review frequency, and communication protocols. In others, the requirements may be structured differently, but the principle remains: your practice needs documented physician oversight to operate legally.
Speed matters here, but speed alone is dangerous. A fast match with the wrong physician—someone whose license does not cover your state, whose specialty does not align with your practice, or whose availability does not match your operational needs—creates more problems than it solves. You may find yourself back at square one during a board audit, or worse, facing questions about patient care with no physician available to consult.
The goal is not just finding any physician quickly. The goal is finding the right physician quickly. That distinction shapes everything that follows.
"Delaying your search for a collaborator is the single biggest bottleneck to your grand opening."
The 7-Day Compliance Sprint to Secure a Supervising Physician Fast
This structured approach compresses what often takes weeks into seven focused days. Each day has a specific objective. Complete them in sequence, and you will move from uncertainty to a confirmed collaboration path before most practices finish their initial research.
Day 1: Confirm the Exact Oversight Requirement in Your State
Before you contact a single physician or service, verify exactly what your state requires. Not all states mandate collaboration, and those that do vary significantly in their specific requirements.
Start with your state board of nursing website. Look for documentation on prescriptive authority, collaborative practice agreements, and supervision requirements. The AANP State Practice Environment resources provide a useful national overview, but your state board remains the authoritative source.
Confirm whether collaboration affects your prescriptive authority. In many states, an NP cannot prescribe controlled substances—or any medications at all—without an active collaboration agreement. Confirm whether payer enrollment or credentialing requires documented physician oversight. Some insurance panels will not process applications without it.
Document what you find. You will need this information when evaluating potential collaborating physicians and when completing your agreement.
Day 2: Build Your Readiness Packet Before You Start Outreach
Reaching out to potential collaborators without your information organized wastes everyone's time and slows down your match. Before you make contact, gather the following:
Your current NP license status and license number
Your malpractice insurance status and coverage details
The state or states where you intend to practice
Your practice type and specialty focus—whether that is general medicine, behavioral health, telemedicine, urgent care, or another model
Whether you will prescribe controlled substances
Your NPI number, or confirmation that you have applied through the NPPES system
Your target launch date
The level of collaboration you need—from active mentorship and frequent consultation to more administrative oversight
Having this packet ready demonstrates professionalism and allows potential collaborators to assess fit quickly. It also reduces the back-and-forth that delays matches. This list mirrors what collaboration services actually request during intake, which means completing it now accelerates every conversation that follows.
Day 3: Set Your Minimum Physician Criteria
Not every available physician is the right fit for your practice. Before you start evaluating options, define your non-negotiables.
The physician must hold an active, unrestricted license in your practice state. This is foundational and non-negotiable. Specialty alignment matters for certain practice types—a behavioral health practice benefits from a psychiatrist collaborator who understands the nuances of that patient population. For more information on why specialty fit matters, see why a generalist collaborator can create risk for behavioral health practices.
Consider communication expectations. How quickly do you need responses to clinical questions? What method of communication works best for your workflow—phone, encrypted text, video conference? Clarify chart review expectations. Most collaboration arrangements include periodic chart review as part of the oversight relationship. Understand what frequency and format works for both parties.
Remember that collaboration may range from very hands-on guidance to less-involved administrative oversight—and that you should have the option to switch physicians if the initial match does not serve your operational reality.
Define these criteria now so you can evaluate options efficiently rather than deliberating with each new possibility.
Day 4: Vet Licensure, Standing, and Practical Fit Quickly
Speed and due diligence can coexist. The key is knowing exactly what to verify and having a systematic approach.
Confirm active licensure through your state medical board's public lookup tool or through the FSMB Physician Data Center. Check for any disciplinary actions, restrictions, or pending investigations. A physician with license complications creates liability exposure for your practice.
Beyond credentials, assess practical fit. Does the physician understand your practice model? Are they responsive during initial conversations? Do they seem genuinely interested in the collaboration, or does this feel like a transaction they will forget about once papers are signed? The physician who ghosts you during onboarding will likely ghost you when you have a complex patient case and need consultation.
A 15-minute phone call can reveal more about practical fit than any credential verification. Make that call.
Day 5: Compare Support Models and Pricing Without Getting Trapped by Speed Alone
With vetted options in front of you, compare what each actually offers. The cheapest monthly rate means nothing if the collaboration falls apart during your first board inquiry.
Collaboration services typically range from approximately $500 to $1,250 per month, though this varies based on practice type, state requirements, and support level. Price alone should not drive your decision. Evaluate what you receive for that price: chart review frequency and depth, consultation availability, response time expectations, and contract clarity.
Ask about the matching process. Some services promise instant matches; others take more care to align specialty and practice model. The article Speed vs Certainty: Why Fastest Match Can Increase Collaboration Risk for NPs explores why the fastest option is not always the safest.
Consider what happens if the relationship does not work. Can you switch physicians without penalty? Is there a process for addressing concerns? A collaboration that looks good on paper but lacks flexibility becomes a liability.
Day 6: Review Agreement Essentials and Launch Dependencies
Before you sign anything, understand exactly what your agreement contains and how it connects to your launch timeline.
A strong Collaborative Practice Agreement or supervision arrangement should clearly define scope of practice, chart review cadence and method, communication protocols, prescriptive authority parameters if applicable, and termination provisions. The article Understanding the Collaborative Practice Agreement: Essential Clauses for Independent NPs provides detailed guidance on what to look for.
Clarify which documents you will receive and when. Some state boards require specific forms. Some payers need collaboration verification as part of credentialing. Know what you need to submit and confirm the collaboration service can provide it in the format and timeframe your launch requires.
If controlled substances are part of your practice, verify that the collaboration arrangement supports your DEA registration requirements.
The distinction between a collaborating physician and a medical director also matters here. These roles serve different functions, and one does not automatically satisfy the other. The article Medical Director vs Collaborating Physician: What Each Role Actually Covers for Independent NPs clarifies when you need one, the other, or both.
Day 7: Submit, Confirm, and Lock Your Next-Step Timeline
Day seven is execution day. Submit your application or quote request. Confirm receipt. And most importantly, clarify exactly what happens next.
Ask for a specific timeline. When will you be matched? When will you receive your agreement for review? When will you have the documentation needed for your board submission or payer enrollment? A vague "soon" is not acceptable when your opening date is fixed.
Provide everything requested promptly and completely. Delays on your end compound delays on theirs. If you prepared your readiness packet on Day 2, this step should be straightforward.
Once confirmed, note the key dates in your launch calendar and follow up if any milestone slips.
Fast Does Not Mean Careless: How to Avoid a Risky Match
The pressure of an approaching launch date can push founders toward shortcuts. A signature-only arrangement that looks like collaboration on paper but provides no real support. A physician who agrees to everything without asking about your practice. A service that promises a match in hours without any vetting process.
These shortcuts create risk that far exceeds any time saved.
Consider the NP who secured a low-cost collaboration agreement just to check the compliance box. Six months later, a routine board inquiry requested documentation of chart review. The physician had never reviewed a single chart. The NP now faced not just the original compliance gap but questions about the validity of the entire collaboration period. The problem that could have been solved properly in a week became a license-threatening situation.
Informal arrangements carry similar dangers. For a detailed examination of why handshake deals and vague supervision terms create exposure, see The Hidden Financial and Legal Risks of Informal Supervisory Agreements for NPs.
The most dangerous mistake is treating speed as the only metric that matters. A fragile arrangement can create a second compliance problem after the first one seems solved. The real failure modes include physician ghosting, specialty mismatch, exorbitant fees, weak oversight, and poor audit defensibility. Those risks become more concrete when the relationship is built around "signature-only" thinking instead of a real support model.
Speed matters. But compliance, fit, and reliability matter more.
What to Have Ready Before You Request a Quote
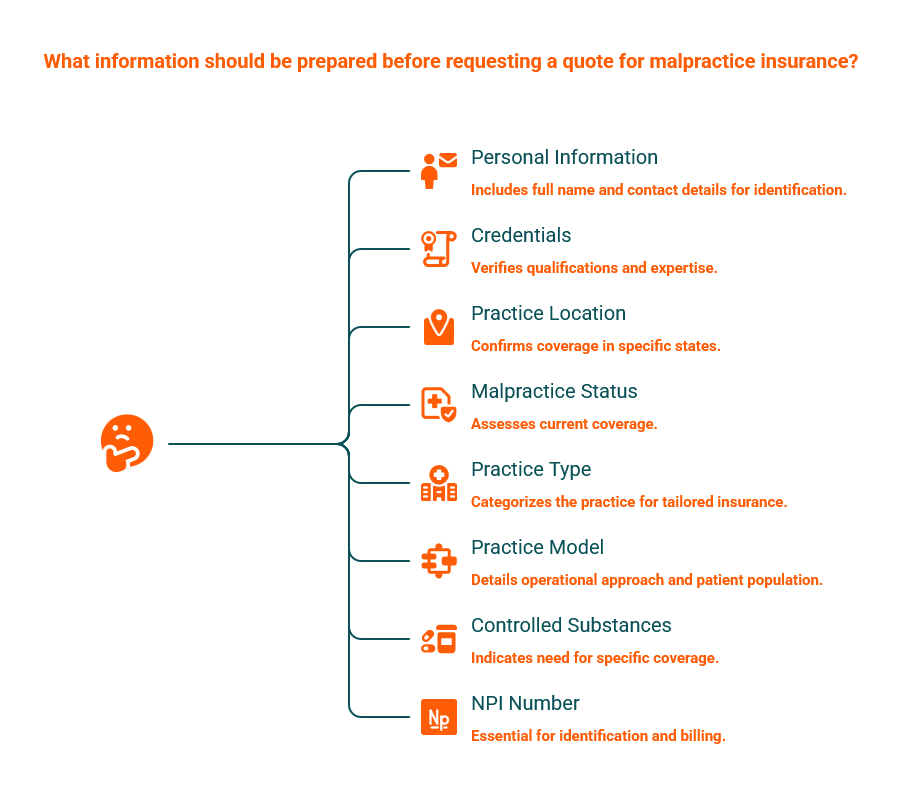
Streamline your intake process by preparing this information in advance:
Your full name and contact information
Your degree and credentials
The state or states where you will practice—confirm current coverage on the States We Cover page
Your malpractice coverage status
Your practice type—general medicine, behavioral health, telemedicine, urgent care, infusion therapy, integrative medicine, med spa, or other
Details about your practice model, patient population, and operational approach
Whether you will prescribe controlled substances
Your NPI number or application status
Having this ready allows the service to assess fit quickly and provide an accurate quote. It also signals that you are a serious, organized practice owner—the kind of client collaboration services want to work with.
Questions to Ask Before You Commit to a Collaborating Physician Service
Before you finalize any arrangement, get clear answers to these questions:
How quickly can you match me with a physician?
Look for specific timelines, not vague assurances. A service that matches within one week provides different value than one that takes a month.
What specialties are available in your network?
If your practice focuses on behavioral health or another specialty area, generic physician availability may not meet your needs.
How will I interact with the collaborating physician?
Understand whether communication happens through encrypted text, phone calls, video conferences, or some combination. Clarify expected response times.
How is chart review handled?
Know the frequency, method, and documentation you will receive. This matters for both operational quality and audit preparedness.
What should I expect to pay monthly, and what does that include?
Pricing clarity prevents surprises. Understand exactly what services are included and what might cost extra.
What happens if the physician is not a good fit?
The ability to switch without penalty or excessive friction protects your practice long-term.
How do you verify physician credentials?
A service that does this work for you saves time and reduces your risk exposure.
These questions filter out services that cannot meet your needs and surface potential problems before they become your problems.
How Physician Collaborators Fits the Launch Window
Physician Collaborators is a network of board-certified physicians with experience collaborating with advanced practice providers. The network includes specialists in Internal Medicine, Family Medicine, Emergency Medicine, and Psychiatry—covering the primary care and specialty needs of most independent NP practices.
The service is designed for the launch-window pressure you are facing. Matching typically occurs within one week. Quote requests receive responses within 24 hours. Once matched, physicians are accessible via encrypted text, phone call, or Zoom conference.
Collaboration can be tailored to your needs, ranging from very hands-on guidance and active mentorship to less-involved administrative oversight. If the initial match does not work for your practice, you have the option to switch physicians. This flexibility protects you from being locked into an arrangement that looked good on paper but does not serve your operational reality.
Monthly pricing typically falls in the $500 to $1,250 range depending on practice type and support level—competitive with industry norms while providing the credential verification and matching support that direct physician outreach often lacks.
Supported practice categories include general medicine, behavioral health, telemedicine, urgent care, infusion therapy, integrative medicine, and med spa, which gives practical context for how specialty fit may show up in real searches.
For NPs launching practices across multiple states, the network's broad state coverage simplifies what would otherwise require managing separate collaborations in each jurisdiction.
Start Now So Compliance Does Not Become Your Opening-Day Bottleneck
The calendar does not care about your compliance gaps. Your launch date is approaching, and every day without confirmed physician oversight is a day of unnecessary risk.
You now have a structured path forward. Seven days of focused action can move you from the vulnerable uncertainty of an empty signature line to the operational security of a compliant, well-matched collaboration. The sprint works. But only if you start.
The cost of waiting is not just measured in delayed revenue—though that cost is real. It is measured in the compounding stress of watching your opening date slip while your competitors see patients. It is measured in the professional credibility lost when you have to explain the delay to staff, landlords, and early patients who booked appointments you now cannot honor.
The cost of action is a few hours of preparation and a single quote request.
Get a free quote from Physician Collaborators and receive a response within 24 hours. Or book a free consultation if you prefer to talk through your situation before committing.
Your grand opening is circled on the calendar. Make sure compliance is not the reason it stays circled longer than planned.
Helpful External Resources: AANP State Practice Environment, FSMB PDC Query, NPPES Apply for an NPI, DEA Diversion Control Division
Disclaimer: This content is for informational and educational purposes only. It does not constitute legal, licensing, medical, or credentialing advice. Requirements vary by state and by practice model; readers should verify requirements with the relevant state board and qualified advisors before making opening or compliance decisions.
Our Editorial Process:
Our expert team uses AI tools to help organize and structure our initial drafts. Every piece is then extensively rewritten, fact-checked, and enriched with first-hand insights and experiences by expert humans on our Insights Team to ensure accuracy and clarity.
The Physician Collaborators Insights Team
The Physician Collaborators Insights Team is our dedicated engine for synthesizing complex topics into clear, helpful guides. While our content is thoroughly reviewed for clarity and accuracy, it is for informational purposes and should not replace professional advice.